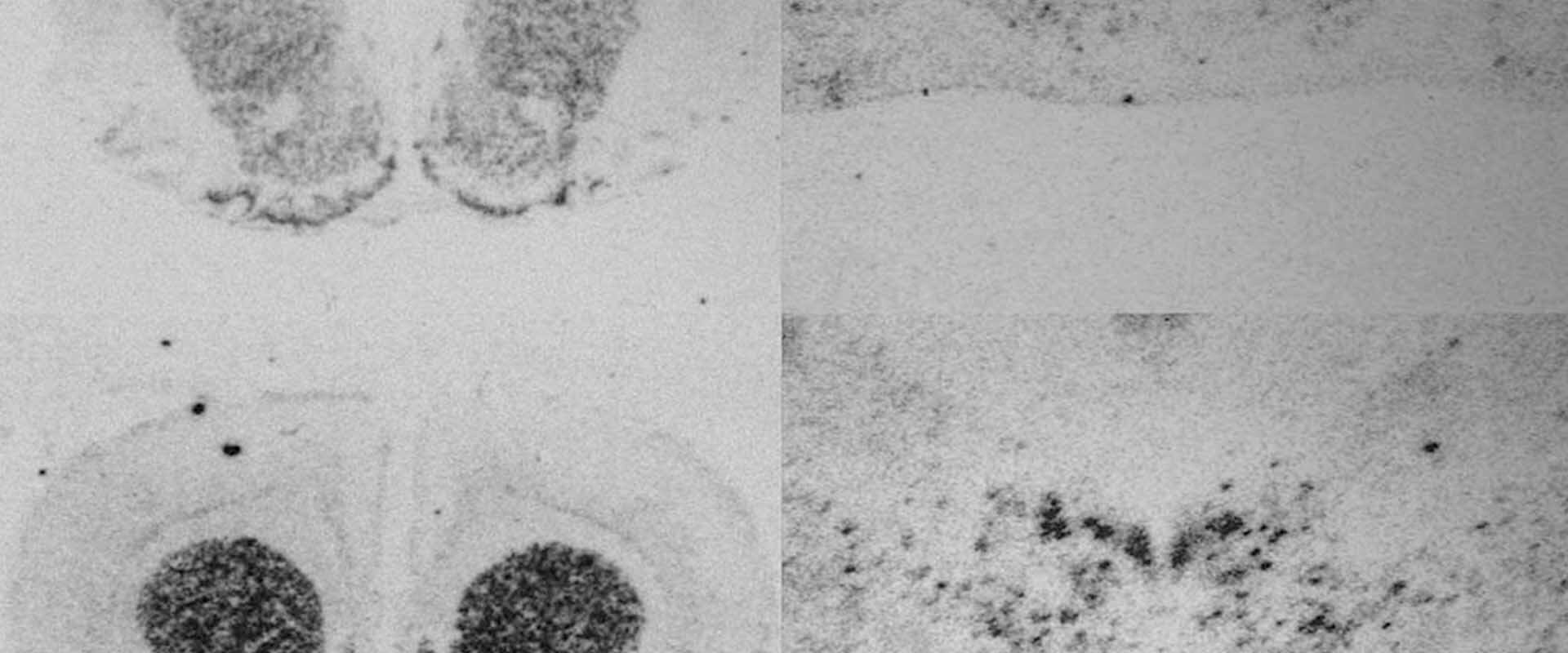
Endocannabinoid system gene expression in mesocorticolimbic brain regions of individuals with alcohol use disorder: A descriptive study.
Researchers at the Institute for Neurosciences UMH–CSIC identify key genetic alterations in the brains of people with alcoholism
• The study, published in the journal Addiction, reveals how decades of alcohol consumption alter the activity of key genes in brain regions involved in addiction.
• The findings help explain vulnerability to relapse and open new avenues for the development of more targeted treatments for alcoholism.
(Photo: IN UMH-CSIC researchers Abraham Torregrosa, María Salud García Gutiérrez, Jorge Manzanares, and Francisco Navarrete.)
Chronic alcohol consumption profoundly alters the expression of genes in the endocannabinoid system in key brain regions, according to a study led by the Institute of Neurosciences (IN), a joint research centre of Miguel Hernández University of Elche (UMH) and the Spanish National Research Council (CSIC). The work, published in the journal Addiction, shows how these changes affect areas involved in reward, impulse control, and decision-making, and opens new paths to better understand the biology of addiction and improve its treatment.
“Alcoholism is one of the leading causes of disease and death worldwide, yet despite its social and health impact, available therapeutic options remain limited”, explains Jorge Manzanares, lead author of the study and head of the Translational Neuropsychopharmacology of Neurological and Psychiatric Diseases laboratory. “That is why understanding what changes in the brain after decades of consumption is key to developing more effective therapies”, he adds.
In this context, the study focused on analysing the neurobiological mechanisms associated with alcohol use disorder by examining post-mortem brain tissue from individuals who had consumed alcohol chronically for an average of 35 years. Specifically, the researchers investigated changes in the endocannabinoid system, which is closely linked to reward and addiction mechanisms.
The endocannabinoid system is a chemical communication network that regulates essential functions such as pleasure, memory, mood, and stress response. It is composed of receptors such as CB1 and CB2, their natural ligands, and enzymes responsible for their degradation, including FAAH and MGLL. “This system acts as a fine modulator of brain function and plays a central role in reward and motivation processes”, explains Manzanares.
Although it was already known that alcohol interacts with this system, there was little evidence based on studies of the human brain. The new work provides a detailed view of how chronic alcohol consumption alters the expression of key genes of the endocannabinoid system in brain regions involved in addiction.
The researchers analysed two core areas of the mesocorticolimbic system: the prefrontal cortex, which is associated with judgement, planning, and decision-making, and the nucleus accumbens, considered the central hub of reward and habit formation.
By comparing samples from individuals with alcohol use disorder with those from non-addicted individuals, the team observed a marked imbalance in the expression of several endocannabinoid system genes. In particular, they detected a strong increase in the CB1 receptor: expression of the gene encoding this receptor rose by 125% in the prefrontal cortex and by 78% in the nucleus accumbens. “This receptor is closely involved in the reinforcement of addictive behaviours and the risk of relapse”, notes researcher María Salud García Gutiérrez, first author of the study.
In contrast, expression of the CB2 receptor gene was reduced by approximately 50% in both regions. “Since the CB2 receptor plays neuroprotective and anti-inflammatory roles, its reduction suggests an impairment of the brain’s defence mechanisms against alcohol-induced damage”, explains the researcher.
Another striking finding was the alteration of the GPR55 receptor, known as an ‘orphan’ receptor because for years its natural ligand was unknown. The researchers found higher levels of GPR55 in the prefrontal cortex, with a 19% increase, but significantly lower levels in the nucleus accumbens, with a 51% reduction. This study is the first to document changes in this gene in humans with alcohol use disorder.
Image: Chronic alcohol consumption alters gene expression of the endocannabinoid system in brain regions involved in reward and behavioral control. Source: IN UMH-CSIC.
In addition, the team observed changes in the enzyme FAAH, which is responsible for degrading anandamide, an endocannabinoid produced by the nervous system that influences anxiety and pleasure. In individuals with alcoholism, FAAH gene expression was lower in the prefrontal cortex but 24% higher in the nucleus accumbens, potentially altering the availability of these regulatory substances.
One of the strengths of the study is the use of brain tissue samples from the New South Wales Tissue Resource Centre in Sydney (Australia). These samples came from individuals with chronic alcoholism who did not consume other illicit drugs, making it possible to isolate the specific effects of alcohol on the human brain without the usual interference of polysubstance use. “This approach provides a clearer picture of how alcohol alone reshapes gene expression in brain regions that are key to addiction”, says García Gutiérrez.
According to the authors, these findings help to better understand why the brains of people with alcohol use disorder show increased vulnerability to relapse and reduced executive control. Identifying which components of the endocannabinoid system are altered, and in which brain regions, opens the door to new, more specific and personalised therapeutic targets.
The authors of the study are also members of the Primary Care Addiction Research Network of the Instituto de Salud Carlos III, as well as the Alicante Institute for Health and Biomedical Research (ISABIAL). The work also involved the participation of researcher Gabriel Rubio from the Hospital 12 de Octubre Health Research Institute (i+12).
This research was funded by the Carlos III Health Institute, the Spanish Ministry of Science, Innovation and Universities, and the Spanish Ministry of Health, within the framework of national research networks on addictions and health, with the support of ISABIAL. The Institute for Neurosciences is accredited as a Severo Ochoa Centre of Excellence.
Source: UMH Communications Service (comunicacion@umh.es) / Institute for Neurosciences UMH-CSIC (in.comunicacion@umh.es)

 Español
Español